Powering the Vaccine Cold Chain (SDG Blog Series)
Shot@Life works to achieve UN SDGs by supporting initiatives to protect deep cold chains required for maintaining COVID-19 vaccines.
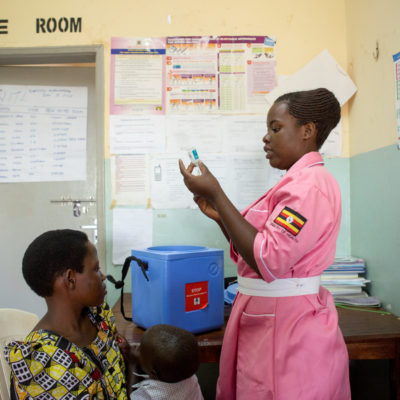
Energy for All
Energy: it’s what powers our earth.
In the U.S., we’ve swapped out our neon lights and fluorescent bulbs for LED ones. Solar panels don the rooftops of countless suburban homes. In many senses, energy almost feels like an unlimited resource: when we want it, we simply plug in our phones to the wall and receive an instant charge. Yet around the world, 759 million people still lack access to electricity.
The seventh Sustainable Development Goal is targeting this issue, focusing on “ensuring access to affordable, reliable, sustainable, and modern energy for all.” Without mentioning renewable energy, the energy crisis around the world extends far beyond the day-to-day conveniences of lighting our homes or energizing our appliances. The United Nations Foundation’s own Clean Cooking Alliance focuses on eliminating polluting cooking fuels like charcoal, wood, and kerosene that many women use to prepare meals. Whether in the form of clean cooking systems or electricity, energy can be a luxury for those living in poverty.
In reality, finding innovative ways to provide clean energy to the developing world has ripple effects in the world of global health, too. Primarily, use cases like the vaccine delivery system and finding innovative ways to keep vaccines cold can ensure that lifesaving vaccines reach the children who need them.
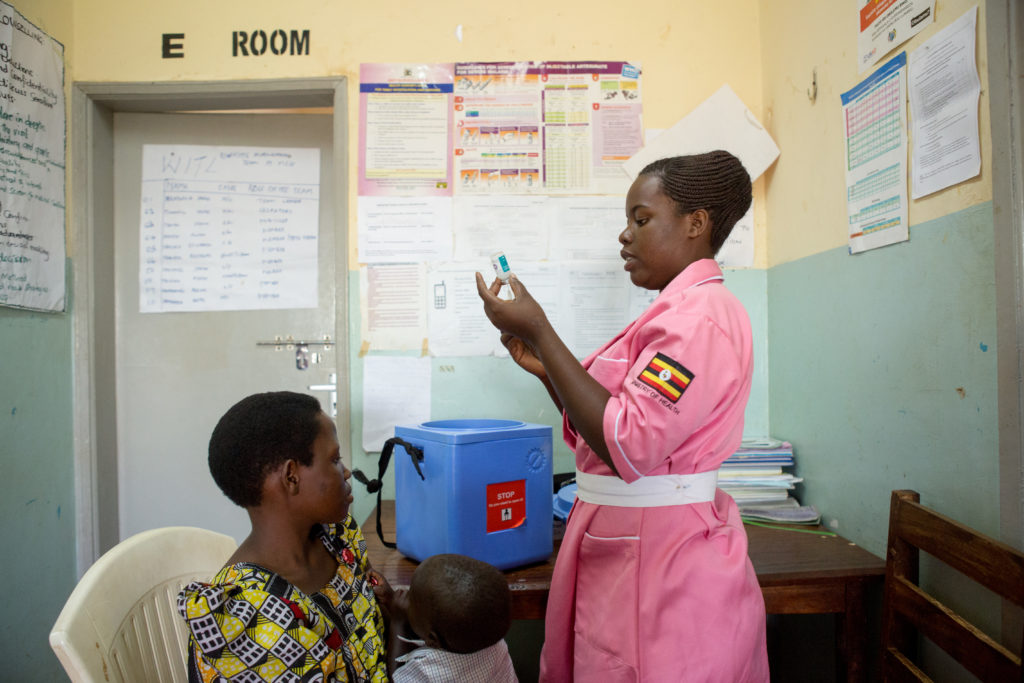
Nurse-midwife Flavia Nambi, 28, prepares to administer a vaccine from a cooler at Nankandulo Health Center IV, in Kamuli District, Uganda.
Powering Vaccine Transport
A few years ago, the UN Foundation featured a story from the Kigambo Health Center in western Uganda. The health clinic — located 10 miles from the nearest power grid — would sit in complete darkness once the sun set. Electricity powers hospitals, medical equipment, and keeps vaccines refrigerated. However, when there are power outages, extreme heat, or other hiccups in the cold chain in rural or remote places, health care systems and services can be severely disrupted.
This is what the Kgambo Health Center struggled with until they were able to install solar panels to the roof of their clinic. But the health center’s previous reality of blackouts isn’t unique for a lot of people. Out of the 759 million people without access to electricity, three out of four of them live in sub-Saharan Africa.
Vaccines are typically stored at temperatures ranging from 35 and 46 degrees Fahrenheit, meaning anything hotter renders them useless. (For reference, a typical refrigerator usually hovers around 40 degrees Fahrenheit.) Due to breakdowns in the temperature-controlled transport and storage system of vaccines, known as the “cold chain,” a lot of vaccines don’t get delivered in the last mile. In fact, according to the World Health Organization, up to half of the world’s vaccines could be wasted each year.

Healthcare on wheels: the Zimbos Abantu mobile clinic carries a stock of refrigerated vaccines to remote communities. It has a wind turbine and solar panels that power the 190-liter vaccine freezer. / Credit: Gavi, the Vaccine Alliance
Dependent on the Cold Chain
It’s not an understatement to say that vaccines are entirely dependent on the cold chain, and even a country’s health system to maintain the right kind of refrigerators to receive them. As we’ve seen with the Pfizer-BioNTech COVID-19 vaccine’s requirement of a “deep cold chain,” requiring dry ice to maintain ultra-cold temperatures for storage (between -90°C and -60°C), this may be difficult for some developing countries that don’t have the right infrastructure. Ultimately, any innovations to secure stable sources of electricity and energy factor into a country’s readiness to successfully receive, deliver, and administer lifesaving jabs.
Although significant progress has been made to ensure global access to electricity, there will still be an estimated 660 million people without access to it in 2030. The COVID-19 pandemic has only impeded this progress. As initiatives such as COVAX roll out COVID-19 vaccines to the entire world — an operation unprecedented in scale and complexity — efforts to power cold chains and health clinics will be more interconnected and important than ever.
