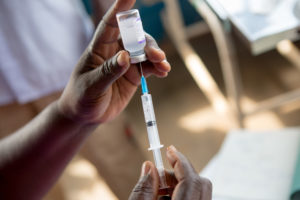
Current COVID Situation
Since COVID-19 reached the US early this year, there has been little room for other topics amidst the discussion of morbidity rates, prevention, and possible vaccinations. As of August, US deaths are over 165,000, while global deaths surpass 760,000. Meanwhile, global confirmed cases have skyrocketed to over 20 million. Unsurprisingly, there is currently enormous pressure on the scientific community to come up with answers, and to produce a vaccine for this novel disease. While our current level of progress is a tribute to the leaders in this field, we still have a long way to go before a viable vaccination will be ready for distribution.
Research & Development
Under normal circumstances, vaccine testing and approval occurs in four distinct stages. Phase I focuses on safety and dosage, and utilizes human subjects to determine the dose of a new drug. Following this, phase II is used to prove the efficacy of the drug. If the drug is proven to be effective, it will move on to phase III, where researchers will decide if any side effects are worth the benefit provided by the medication. Once a drug passes this stage, it can be approved by the Food and Drug Administration (FDA). Phase IV serves to continually monitor the drug as it is used to treat hundreds or thousands of patients. This final stage allows scientists to study both the short and long-term effects of the therapy. This process normally takes anywhere from 10 to 15 years. However, waiting this long to put a vaccine for coronavirus on the market could have disastrous effects.
The current administration has developed Operation Warp Speed (OWS) to help respond to this extremely time-sensitive challenge. The official aim of this ambitious project is to deliver 300 million doses of a viable COVID-19 vaccine by January 2021. The main effect of this project is to accelerate trial vaccines through the normal research and development (R&D) process. However, another important aspect is to establish manufacturing and distribution capabilities before a vaccine is approved, so that it can be provided to those who need it most as soon as it is approved by the FDA. $10 billion has been contributed to this monumental effort, and Congress is in the process of appropriating additional funding. Worldwide, there are currently over 165 possible coronavirus vaccinations being studied. However, pharmaceutical companies AstaZeneca, Johnson & Johnson, Merck, Moderna, and Pfizer are the five finalists who were chosen in June to receive funding from the OWS initiative.
Actors & Timeline
Johnson & Johnson has started human trials in Belgium on its SARS-CoV-2 vaccine. Merck, the only company to successfully develop an Ebola vaccination, is also currently transitioning into human trials. The three vaccinations that are furthest along in the R&D process are Moderna’s mRNA-1273 vaccine, AstraZeneca’s AZD1222 vaccine, and Pfizer’s BNT 126 vaccine. Through Operation Warp Speed, the US government pledged to fund the phase III trials for each of these most promising coronavirus vaccinations. These phase III trials will be the most involved developmental step yet, and will utilize tens of thousands of subjects at many sites around the US. AstraZeneca’s phase III study in Britain could be completed as early as August. In the United States, Moderna was the first vaccine to begin phase III trials in late July, and is expected to enroll 30,000 healthy adults who do not have COVID.
While there is a clear risk in waiting to produce a coronavirus vaccine, there are also risks in speeding up the R&D process in this way. One clear example of this is the drug hydroxcholoroquine, which was approved by the FDA as a COVID treatment back in March. However, this authorization was revoked early this week following a lack of efficacy evidence. Moreover, hydroxcholoquine’s temporary use was associated with over 400 adverse events, including 109 serious cardiac episodes. Had normal protocol been followed, this drug would have never been on the market before these issues were detected.
Leaders in health around the world are working to balance the risks of unveiling a vaccine early with the risks of waiting. While this issue is evolving every day, several prominent health-oriented groups are publishing pieces on the risks and benefits of rushing the R&D process. Most prominently, the WHO recently released a comprehensive document that is meant to help researchers navigate these ethical issues.
Looking Ahead
Despite all of this progress, the question of when a vaccine will be ready still remains. Unsurprisingly, different members of the scientific community have different estimates. Recently, Dr. Anthony Fauci of NIAID claimed that there could be “tens of millions” of vaccine doses available in early 20201. Other groups of experts assert that a more likely distribution would be in the summer or fall of 2021. However, it is important to remember that these are just educated guesses, and that researchers will have much more information following the completion of the impending phase III trials.
As of now, the United States and the world appear to be heading full tilt towards a vaccination approval in the near future. However, the ethics of rushing this complicated process are still up for debate. What is certain is that we are currently in the midst of a rapidly evolving pharmaceutical race for the cure, and that the government and the scientific community are under extreme pressure to produce fast results. The vast majority of professionals agree that a vaccine will be the ultimate solution, but the timeline and the treatment have yet to be decided.
If you are passionate about Shot@Life and vaccine accessibility, please consider taking action or donating.
Updated August 14, 2020
